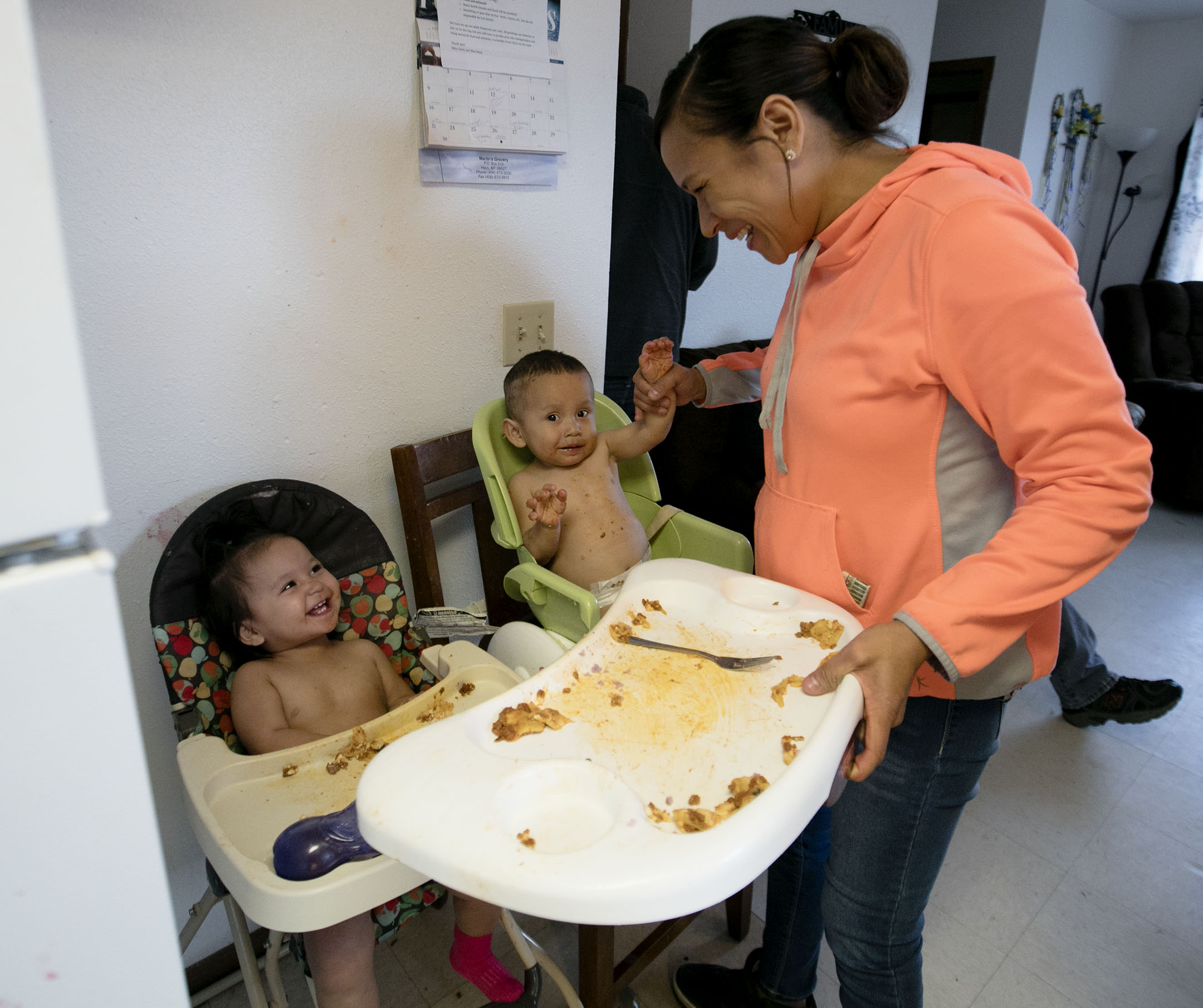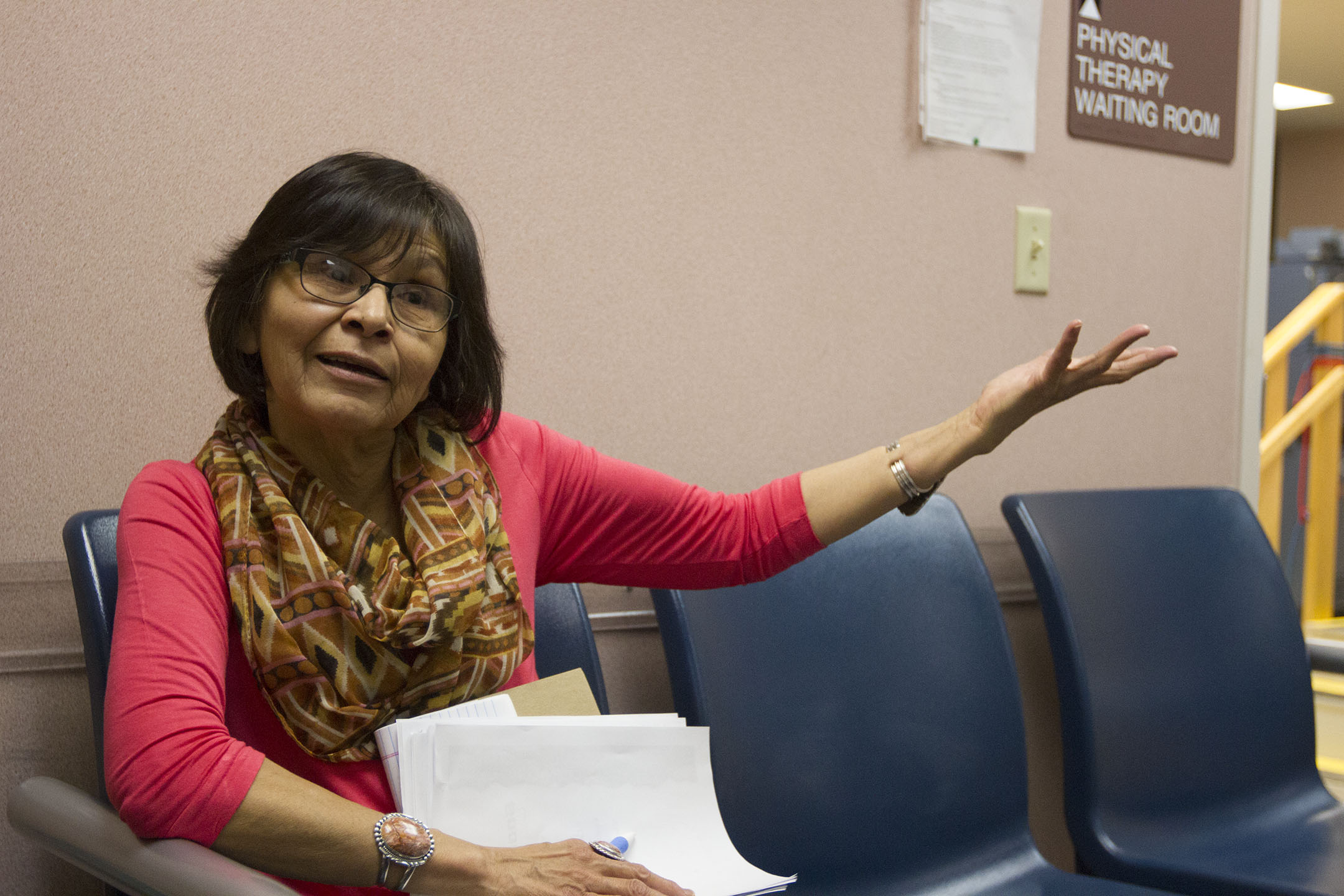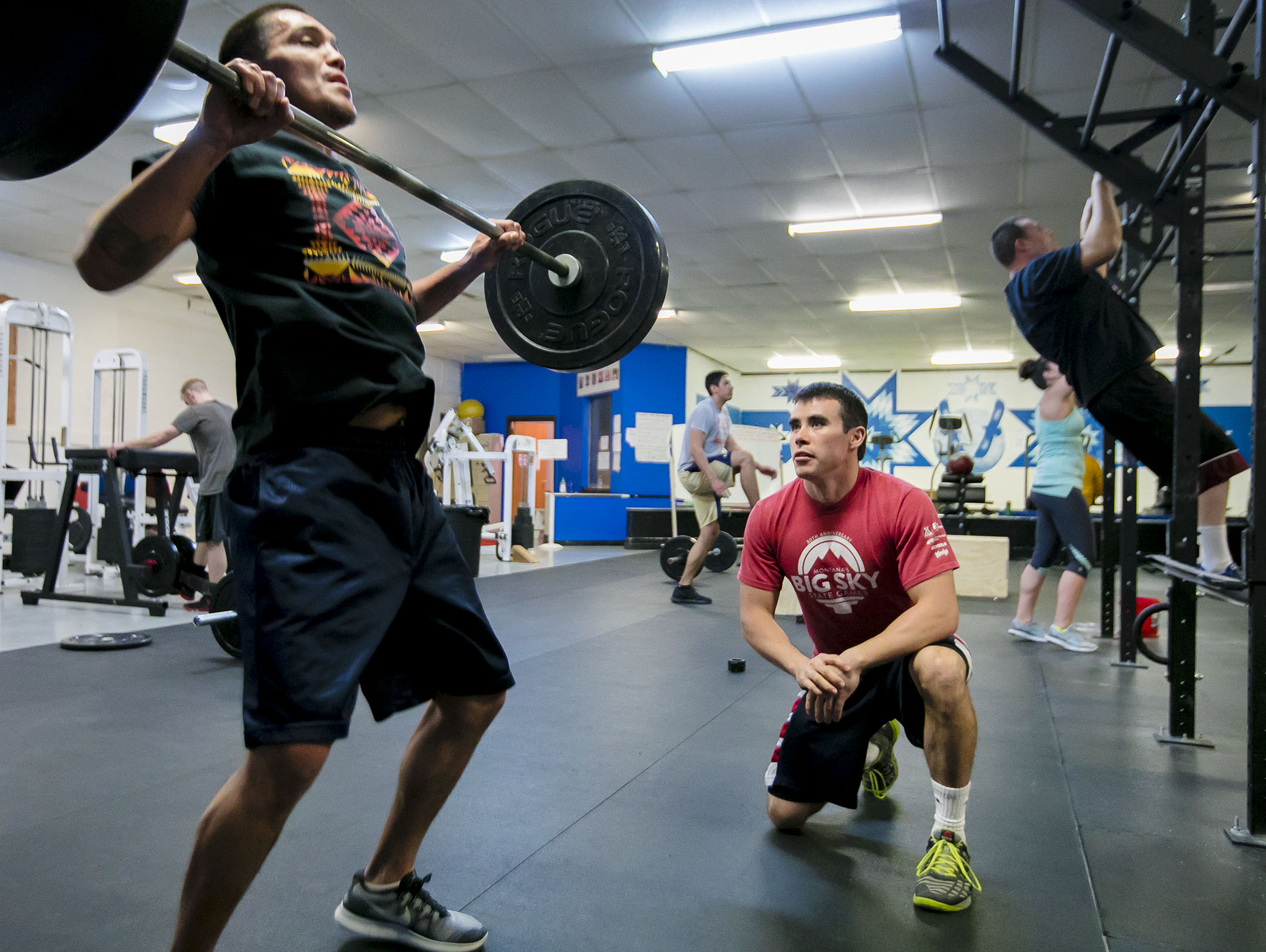Story by Lucy Tompkins, photos by Adam McCaw
When Jean Bear found out she was pregnant, she did what all women in Hays, Montana must do: She drove 82 miles across the Fort Belknap Indian Reservation to the nearest hospital with prenatal care and delivery services for her first checkup.
Her route took her past Fort Belknap’s Indian Health Service, the facility created to provide health care to the reservation’s tribal residents, as mandated by treaties between tribes and the federal government. Fort Belknap IHS stopped delivering babies in the 1970s, so Bear continued 50 miles farther to Havre, where a doctor did an ultrasound and gave her the good news: She’d be giving birth to twins.
Having twins is considered high-risk, so Bear was referred even farther from home for care. She drove to Billings — six hours round trip — for monthly prenatal appointments. Because the Billings hospital is beyond the reservation’s borders, Bear’s treatments and travel costs weren’t covered by IHS, which doesn’t charge Native American patients for care. Without health insurance, Bear would have to pay out of pocket for her monthly appointments, travel and lodging in Billings. As her due date approached, she had to make the 336-mile trip every week.
To cover those costs, Bear signed up for Medicaid. Because IHS doesn’t deliver babies on the reservation, all pregnant women are urged to enroll, as Medicaid reimburses for travel expenses and pays for all medical needs. Nearing her due date, Bear spent three weeks in Billings at a Ronald McDonald House and two nights in the hospital. She doesn’t know how much these costs amounted to, because Medicaid covered them, but the average cost of one night in a hospital in Montana is $1,284, according to the Kaiser Family Foundation. After always relying on IHS for her health care, and never getting the comprehensive treatment she needed, Bear realized how much freedom Medicaid granted her.
Enlarge

Far from her rural hometown of about 800 people, Bear gave birth to fraternal twins, Kale and Hazel. When Bear or her now 16-month-old twins need to see a doctor or a dentist, she doesn’t bother with IHS. She drives her children to Helena for dentist appointments, nearly five hours away. With Medicaid, Bear has access to high-quality care off the reservation, freeing her from the constraints of IHS’ tight budget.
“(Medicaid) gets you faster appointments, and you don’t have to wait around for IHS to go to the board and read on it,” Bear said. “I have really bad asthma, and all I have to do is call and make an appointment. I don’t have to wait around for IHS to schedule me one.”
~-~
Despite the federal government’s treaty responsibility to provide Native American tribes with health care, services on the reservation have long been underfunded. When IHS doesn’t have the resources for a certain procedure, a board of administrators decides if IHS will pay for the patient to receive treatment in a hospital off the reservation — known as contract care. In the past, only patients at risk of losing their lives or a limb were granted that permission, due to lack of funding.
Because IHS has always been the main source of health care on reservations, applying for insurance or Medicaid is foreign to many Native Americans. Some don’t have access to a computer to sign up, and others think it’s expensive. Some refuse to enroll on principle to hold the federal government accountable for its failure to comply with treaty-mandated responsibilities and promises.
After suffering through years of chronic underfunding, IHS has been thrown a lifeline. Both the Affordable Care Act and Montana’s Medicaid expansion provide a new way for IHS to improve its services and increase its revenues. A patient covered by Medicaid allows IHS to bill the federal government for the services it already provides. Currently, the federal government reimburses 100 percent of those expenses. Before the Medicaid expansion, it reimbursed just 65 percent. On the Fort Belknap Indian Reservation, those reimbursements have reached beyond the IHS facility and into the community, improving services and creating stronger preventative health programs.
Greg Smith, acting CEO of Fort Belknap’s IHS facilities, said they are seeing more patients with third party coverage than ever before in its history. The amount of money collected from billing Medicaid, Medicare and private insurance has increased by 15 percent since 2015, he said. Those reimbursements have helped the hospital add more nursing positions and buy new medical equipment to replace antiquated, 20-year-old machines. They’ve also helped departments fund preventative health care services like the community gym.
Nationwide, third party billing at IHS has increased by $240 million, about 26 percent, since the passage of the Indian Health Care Improvement Act, which is included in the ACA.
If the ACA and Medicaid expansion are repealed, that 15 percent budget increase, and the expanded health care options that kept Bear from going into debt to give birth, would go away.
In 2012, Montana had the highest rate of uninsured Native Americans in the country, at 40 percent, according to a report by the National Indian Health Board and North Dakota State University. But since Montana’s Medicaid expansion went into effect in 2015, nearly 10,000 Native American patients have gained coverage.
The expansion made Medicaid available for all adults with incomes up to 138 percent of the federal poverty level ($16,394 for a single adult in 2017). Mark Trahant, an expert on Native American politics, said the expansion makes nearly every tribal member eligible for Medicaid.
“You’re out of luck if contract care runs out of money, but if you have insurance, you get that care,” Trahant said. “The main reason to do it is it’s better for everybody. If more people are insured, the clinic will have more resources.”
~-~
The benefits of third party billing spill beyond Fort Belknap’s IHS hospital, down the road and into the Red Whip Gym. From the outside, the gym looks like a dilapidated, windowless warehouse. Inside, a colorfully painted entryway serves as a portal to a renovated fitness room, basketball court, pool and kitchen for serving after-school meals to kids.
Miles Werk, 26, sits behind the front desk and admits members between the fitness classes he teaches. He recently instated a $1 daily entrance fee for kids, and $2 for adults. In the after-school rush, kids who can’t afford the fee pick up trash outside the gym or do a quick fitness exercise with Werk as a substitute for the money. He won’t turn away a kid who shows up without a dollar, but he wants to teach them to care for the property and for their health.
After graduating from the University of Montana with a degree in health and human performance in 2012, Werk, now the Red Whip Gym recreational fitness and wellness coordinator, returned to Fort Belknap to improve the community gym and teach kids healthy habits.
Enlarge
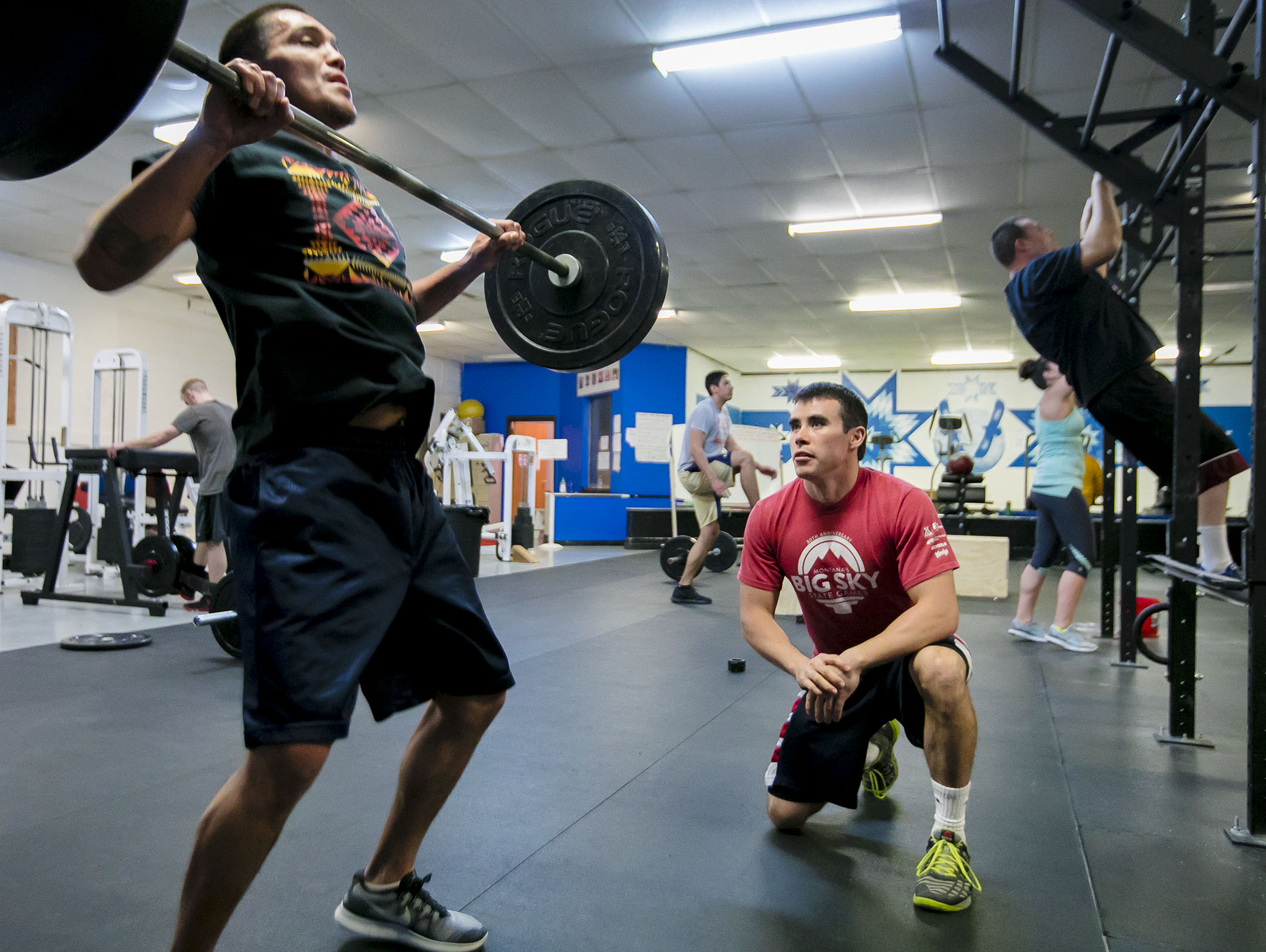
Since his return, the gym, which also serves as a community center for wakes, funerals and events, has transformed. The basketball court, where college basketball games are held and groups of schoolchildren scrimmage after school, has new hardwood floors that replaced the former tile floors from the 1970s.
There’s new exercise equipment: stair steppers, rowing machines, bikes, dumbbells. The pool has a new lining, which replaced the chipping paint that used to float around and clog the filtration system.
A brand new wooden sauna steams poolside.
“People come in and are amazed by the change,” Werk said.
When Werk wants to improve a part of the gym, he has to lobby the tribal government for funds. But lately, he has another source of revenue: Fort Belknap’s Public Health Nursing Program.
The program comprises of eight nurses who do immunizations, home visits, community education, school screenings and more throughout the reservation. Their department is part of the IHS hospital, but it is tribally run. When a patient covered by Medicaid comes to them for treatment, the program can bill for a 100 percent reimbursement.
The program’s manager, Kathleen Adams, said they use Medicaid reimbursements to boost the budget and fund new health equipment like wheelchairs, crutches and gym equipment. In its first contribution to the Red Whip Gym, Adams’ program, along with two local diabetes programs, allocated $14,000. Adams said it can purchase equipment as long as it improves someone’s health.
As a focal point for the community, the improvements to the gym have far-reaching impacts. Werk said more young adults have been taking advantage of the renovated gym, and it dramatically expanded fitness options for kids who don’t get enough physical activity in school. In a place where diabetes rates are more than twice that of non-Native people in Montana, access to a gym and fitness equipment is particularly important.
In addition to its contributions to the gym, the Public Health Nursing Program funds medical equipment for people throughout the community. The program uses Medicaid reimbursements to help those who don’t qualify for Medicaid but can’t afford the medical equipment they need.
Kermit Horn is one such patient. Horn uses a wheelchair, as his legs are paralyzed from having polio as a child. For years, he swung himself along using crutches, but when his doctor warned him of the damage it would do to his shoulders, he switched to a wheelchair. Getting around since then hasn’t been easy, as the reservation isn’t required to comply with Americans with Disabilities Act requirements, and many buildings aren’t wheelchair-accessible. He can maneuver over small curbs while holding a door open for himself and isn’t uncomfortable calling the police on someone who parked so close to a doorway that he can’t squeeze by in his chair.
Horn’s monthly disability check for $1,400 makes him ineligible for Medicaid. When his wheelchair started to tear in the seat and the back, Horn went to IHS to apply for a new one through Medicare. They denied his request, saying the chair wasn’t in bad enough shape.
Enlarge

“The seat is about ready to come through,” Horn said, gesturing to the visible rips beside his hips.
He improvised a temporary fix.
“I took it upon myself,” he said. “You see this leather strap? Like you find on the saddle of a horse. I cut four strips and I put them underneath my seat so it wouldn’t completely tear off.”
Without the leather straps, Horn says his seat would have ripped through a long time ago. When Medicare rejected his request for a new chair, the Public Health Nursing Program stepped in and ordered him a new one. It’s on its way. Medicaid reimbursements augmented the program’s budget enough to free up money that can be used to help more people like Horn.
“Without them, a lot of people would be hurting,” Horn said.
~-~
Despite the benefits of enrolling in Medicaid, many Native Americans who are eligible for coverage remain uninsured. One reason for this could be a misunderstanding aboutthe role of IHS, which was created to provide health care for Native Americans but doesn’t constitute health insurance.
Of the roughly 70,000 Native Americans eligible for reduced-cost or free coverage in Montana, only about 17,000 have signed up. Another roughly 22,000 appear to have private insurance through their employers, according to an analysis of state and federal enrollment records by the Billings Gazette in September 2016.
For some, refusing health coverage is a conscious sacrifice with a political message.
Avis Spencer has worked for the environmental health department in Fort Belknap Agency for eight years. She chooses not to purchase the tribe’s employer insurance to hold the federal government accountable for its trust responsibility to provide Native Americans with health care. Health care, housing and education were promised to tribes in exchange for huge swaths of their land, and Spencer doesn’t want that to be forgotten.
“I believe in holding them accountable for that, so I rely on Indian Health Service for my care,” Spencer said. “Good or bad, it’s there, and a lot of people nationwide don’t have that to fall back on.”
Spencer’s choice to forgo health coverage hasn’t been a problem for her, she said, knocking her knuckles on a nearby table, because she hasn’t had serious medical issues that IHS can’t treat. But management of IHS funds has disappointed her, and she compared the hospital to a walk-in clinic, without physical therapy, a well-child clinic for school kids or regular screenings for young men.
Enlarge
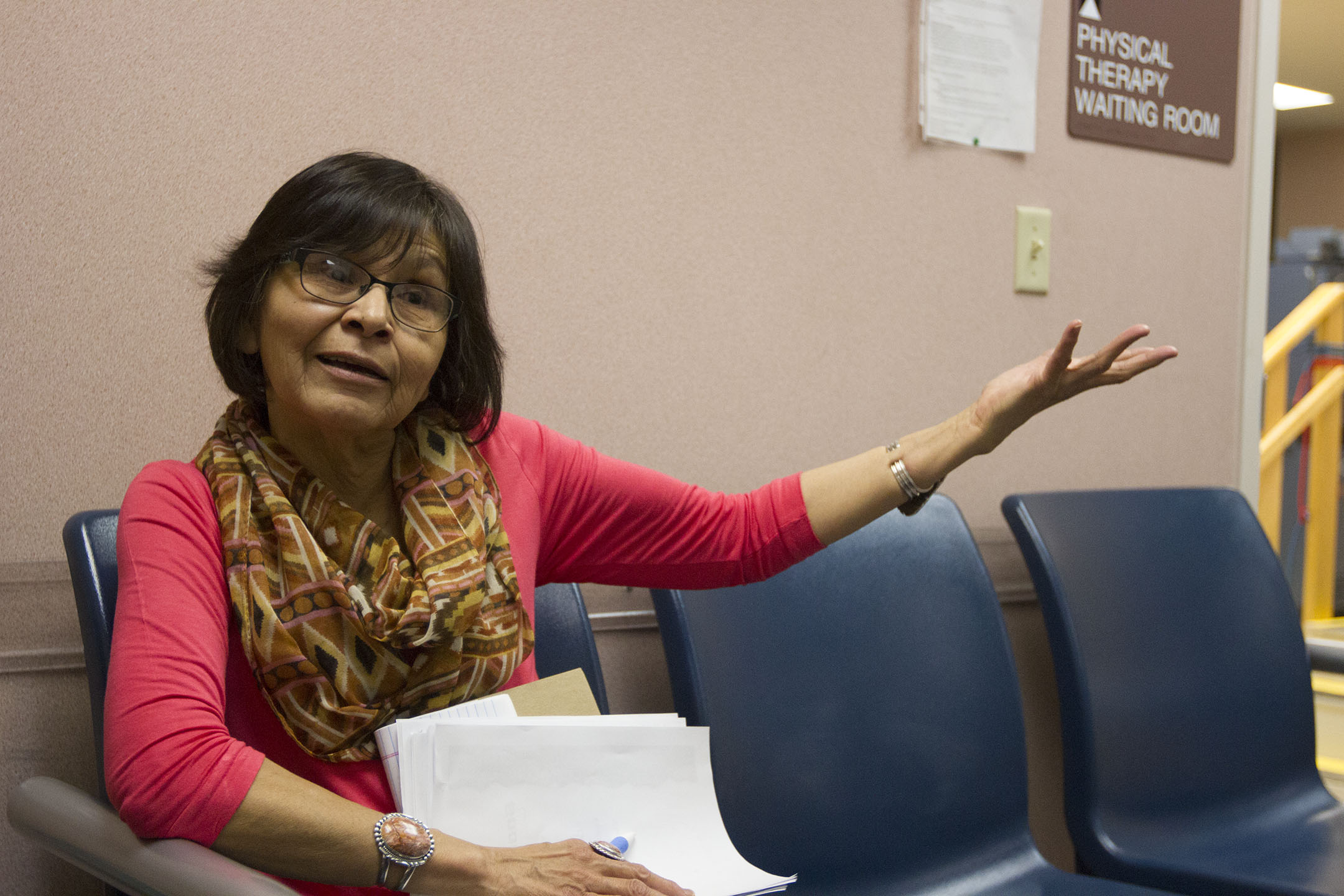
She suggested that rather than continue providing substandard services, IHS funds be given to the tribe to help every member register for health insurance.
“If you can’t provide health care, then give us the money and we can get our own health insurance, rather than just being here and providing jobs,” Spencer said, adding that the jobs are helpful for tribal members, but most providers come from outside the reservation.
Of three permanent health providers and a handful of contracted providers at the IHS facility, only one is from the reservation.
~-~
Other people who remain uninsured have simpler reasons. In March, a new program launched to help register people on the reservation for Medicaid. Theresa Sullivan, the outreach worker for Hays and Lodgepole, visits homes and attends community events to find the people who have slipped through the cracks, she said.
So far, she’s helped 13 people sign up. The biggest barriers she’s seen are a lack of internet access and a misunderstanding about the benefits of insurance. Until Montana expanded Medicaid and the ACA required employers like the tribal government to provide health insurance, IHS was the main option for health care on the reservation.
“They don’t have an email, so in order for me to even enroll them I have to make them an email,” Sullivan said. “Or use my own, I guess.”
In a few instances, people haven’t wanted to create an email account, so they trust Sullivan to use her own. At a workshop for young mothers in the Kills at Night Recreation Center in Hays, Sullivan made her rounds with a notebook and pen. Various speakers educated new or soon-to-be mothers about breastfeeding, nutrition and other care-taking practices.
Sullivan spoke to each woman between speakers to share the benefits of Medicaid and to enroll the uninsured. She recorded each mother’s contact information on her note pad. She knew nearly everyone present, as is the case in such small towns.
Though Sullivan’s job is to spread the word about Medicaid and the benefits of health coverage, she remains uninsured. The insurance provided by her employer, the tribe, is too expensive for her to afford, but she’s not eligible for Medicaid as a one-person family with a decent income. She relies on IHS.
“I can’t claim my dog,” she said, giggling. Still, she’s happy to be helping other families enroll.
“A lot of these people are low-income, and I’m sure if I really scrimped I could afford insurance,” she said. “But I like it. I’m glad that they can have better health care. Especially for the kids, because they really need it.”
~-~
Widespread complaints about IHS are often followed by a sympathetic concession: For how little money it has to work with, the care it provides could be worse.
Though IHS funding saw some increases under the Obama administration, tribal leaders aren’t expecting the same treatment from President Donald Trump. But as long as the ACA isn’t repealed and Medicaid expansion continues to exist in Montana, IHS has a way to build its own revenues without relying on Congress. Third-party billing gives IHS the freedom to bill the government for funds they’d otherwise never see, for procedures they’d otherwise provide at no cost.
The revenue possibilities, if all eligible Native Americans enrolled for coverage, would be drastic. While the Fort Belknap IHS hospital has already begun to benefit from newly insured patients, that growth won’t continue if insured patients prefer to seek care outside the reservation. For Bear and her twins, it makes more sense to drive the extra miles for better care than to wait for approval or rejection from IHS, which has limited funds.
Enlarge
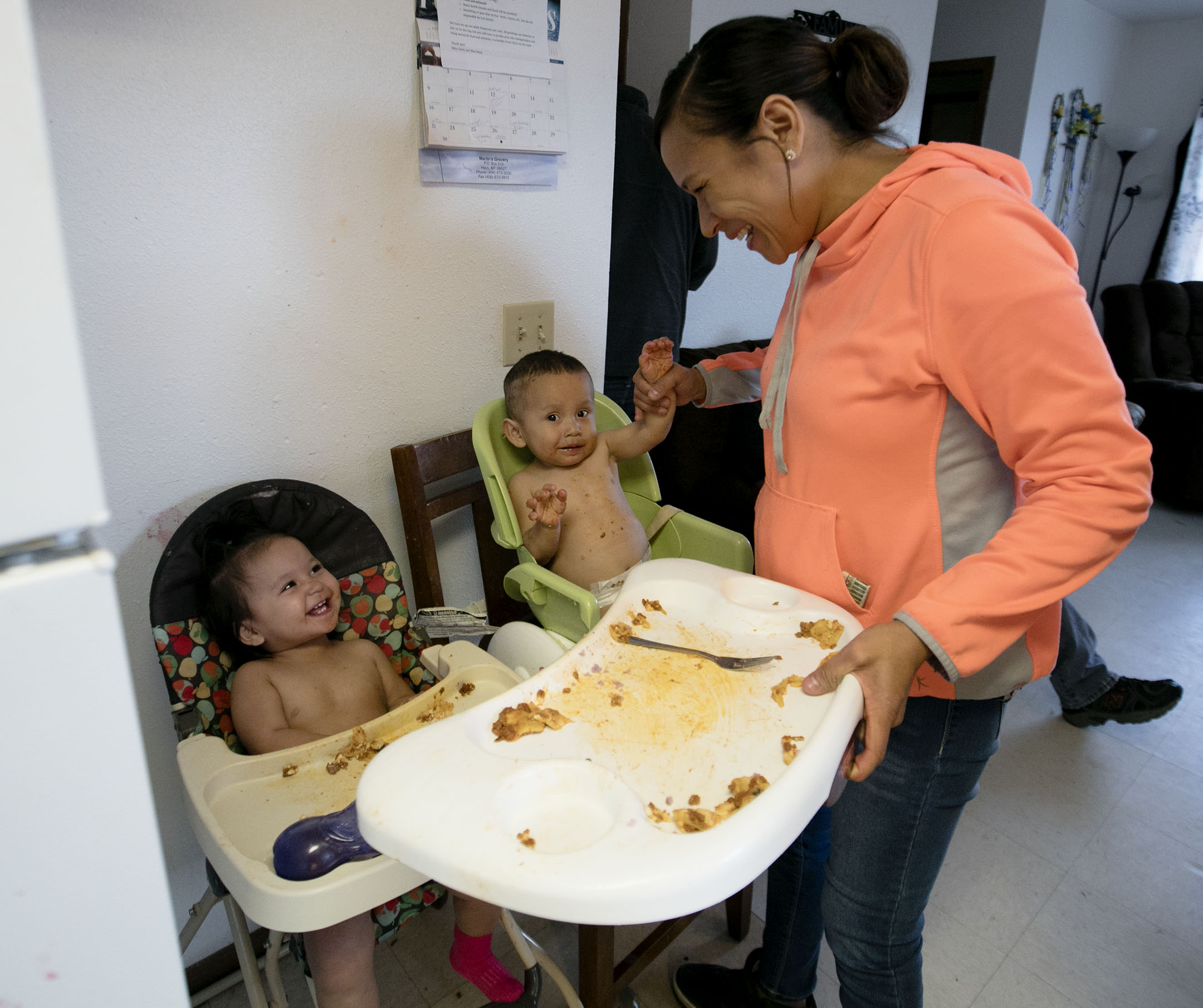
But Tribal President Mark Azure argues that people should always come to IHS first so that the facility can build itself up little by little. By encouraging people to make IHS their primary provider, Azure hopes that one day the facility will have a physical therapist again, and more resources for behavioral health so that in time, his people will get the best quality care.
“I believe that we are creatures of habit, and the ability to take an hour off from work and walk over here,” Azure said, pointing out his window to the IHS hospital, “rather than take a whole day and drive to Billings if you don’t have to — whether it’s snowing, raining, whatever the case — we’re gonna start coming back to this thing, and eventually it’ll all pay off.”
Smith, the acting CEO of Fort Belknap’s IHS facilities, echoed this sentiment.
“The bottom line is, as you can tell, we’re fairly isolated,” Smith said. “And the reality is most people, at some point in time, are going to, just for convenience, come here.”
For Bear, quality currently outweighs convenience.
~-~
In Montana’s remote northcentral plains, Fort Belknap residents have more health care options than ever before. But with the ACA on President Donald Trump’s chopping block, and Medicaid expansion at risk, that freedom and access to quality care could disappear. A complete ACA repeal, according to experts, would regress IHS to the days when only patients at risk of losing their lives or a limb were sent to a hospital outside the reservation.
In her 10 years working for tribal health, Assistant Director Tammy Rider has seen the difference insurance makes. Those who have Medicaid or insurance from the tribe have elevated their health care, and they have options and more control over their own health. But for those who haven’t, or can’t afford to, IHS continues to be their only hope. Unless IHS reaps the benefits of Medicaid reimbursement and helps tribal members enroll for insurance, health care on the reservation will remain inadequate, trapping tribal members indefinitely with second-rate care.
“For the ones who can’t enroll,” Rider said, “they’re just stagnant.”
For past Native News editions visit the archive here.