Story by Nick Callahan, photos by Derek Minemyer
It’s almost idyllic; the modest, sky blue home that stands on the side of a hill, watching the highway run into the horizon. Behind Jay D Old Mouse’s house are empty horse corrals. There has been no sign of horses grazing the land, or running the hills in months.
Extending from his front door is a makeshift wheelchair ramp constructed of loose boards and covered with a long rubber mat. The ramp leads directly to his truck.
Inside, Old Mouse navigated the narrow hallways of his small house with his wheelchair, weaving between his living room and his kitchen. He wheeled himself to the threshold of his bathroom, demonstrating how the tight quarters don’t fit his wheelchair. He climbed out of the chair, clenching the bathroom doorway, showing how he squeezes into the shower.
“When I lost my first leg, simple tasks were a challenge. Cut your leg off and just see,” Old Mouse said. “And to lose the other one becomes a double challenge.”
Old Mouse was diagnosed with diabetes at 28 years old, and has been coping with the disease for more than two decades. It’s a condition in which patients and doctors try to avoid the worst case scenarios, of which there are plenty. In 2016, he found himself in one of those worst case scenarios. Twice.
In March, the doctor said they had to take his leg.
In September, they had to take the other one.
Diabetes has long been an epidemic on Indian reservations, with Native Americans having the highest rate of type II diabetes in the United States. It’s a well-known problem. It’s also well-known that diabetes is preventable, and its symptoms curable, by instilling major lifestyle changes. However, because the Indian Health Service is a medical care organization, most of its funding has been focused on treating symptoms of the disease after it’s been contracted.
But tribes like the Northern Cheyenne, in southeastern Montana, are debating the best methods to fight the disease. It’s a conversation that can be seen in two competing tribal proposals. One is a tribal dialysis center, which would treat patients with varying levels of kidney damage, another diabetic worst case scenario; the other is a community gym, touted as a strategic maneuver to help instill active lifestyles in an effort to prevent diabetes.
Some say the proposed gym would have more value in the long-run, as a dialysis center would passively condone the spread of diabetes. However, patients say a tribal dialysis center is desperately needed. It is literally a life sustaining necessity.
“Looking at the generation coming up, where we have high rates of obesity already and diabetes in our children, we don’t want to be setting them up to fail, but that’s what we’re doing,” said Jace Killsback, Northern Cheyenne tribal president. “I can serve 30 dialysis patients, or I can serve 300 youth, or 3,000 residents here for a nice community and fitness center that would also address dialysis prevention.”
~-~
The story of type II diabetes, a version of the disease that is contracted later in life, in Indian Country is not new. Prevalence of diabetes is highest among Native Americans with a rate of 15.9 percent, according to the American Diabetes Association. This is more than double that of whites
The disease, in which the body stops properly burning sugars digested in carbohydrates, can yield a number of symptoms and health ailments as those sugars build up within the body’s systems over time. Symptoms range from mild, dizziness, frequent urination, to severe, including blindness and kidney failure.
However, diabetes is unique in that patients often have the ability to treat it into remission. It’s a continuous battle in which patients must consistently monitor diet to maintain blood sugar levels, regularly take the prescribed medications and live an active lifestyle.
Enlarge

Yet, most reservations are rural and considered “food deserts,” where fresh produce is expensive and scarce. Patients must rely on a crowded and underfunded IHS system, and community development focuses on essential projects, which usually doesn’t include gyms or outdoor recreation facilities.
About 44 percent of the Northern Cheyenne population is younger than 20 years old, according to the United States Census Bureau. With such a large youth population to consider, Killsback is taking aim at the long-term outlook of diabetes.
He estimates it would take about $700,000 to build a dialysis center in Lame Deer. If the tribe were to make an investment of that magnitude, Killsback said he wants to make the greatest impact possible.
Building a fitness center would leave those 30 dialysis patients in dire straits. It’s a difficult decision and Killsback knows it. But, after decades living on the reservation, he also knows the effects of diabetes.
~-~
It began with black spots on his feet, then the ulcers appeared. Old Mouse’s legs eventually became infected and had to be amputated, or he likely would have died, he said.
After the ulcers appeared on his foot, Old Mouse saw a doctor in Billings that suggested stem cell treatment on his feet, to regrow the skin. But IHS denied the treatment three times, each time calling it experimental treatment, Old Mouse said. He still wonders if the treatment could have saved his legs, had IHS approved it.
“Let’s try it, maybe I could’ve still had my legs. Maybe it would’ve worked and I lost them anyway, but at least try,” Old Mouse said. “Don’t just deny it. They’re not God.”
IHS paid $19,000 for a prosthetic for his left side. He’s still waiting for a right one to match, and he’s hoping IHS will pay for that one as well. If so, IHS will spend nearly $40,000 for both of Old Mouse’s prosthetics.
Enlarge

IHS has a budget of about $4,000 per person per year. The national average spent by health care on patients is twice that, at $8,000 per person per year. While IHS broadly touts its efficiency with such limited resources, efficiency doesn’t always translate to quality care.
After the infection in Old Mouse’s legs, his doctor told him his kidneys were functioning at about 15 percent. They are failing, and fast. Old Mouse is in a pre-dialysis stage, and he hasn’t come to terms with it yet.
“I’m still in good spirits about my legs, but not in good spirits about dialysis,” Old Mouse said. “Dialysis is a game changer.”
There are currently 30 people on Northern Cheyenne who need dialysis, up from 18 in 2010.
Type II diabetes is the leading cause for kidney failure in the United States. High blood sugar over time diminishes the kidneys’ ability to filter and clean the blood. The most common form of dialysis is hemodialysis, in which a patient goes to a clinic and is hooked up to a machine. Blood is lead via catheter out of the body and into the machine, which acts as the kidney and filters the blood before another catheter leads it back into the body.
About half of all diabetes patients experience some form of nerve damage, according to the American Diabetes Association. Nerve damage in the feet can be especially problematic. It can cause loss of feeling in the feet, which makes it harder to detect sores that can easily become infected. In 2010, there were 73,000 lower limb amputations in diagnosed diabetes patients over the age of 20, according to the American Diabetes Association.
Dialysis patients on Northern Cheyenne must commute more than 100 miles to Billings three times a week for treatment. The commute can take its toll.
~-~
It’s just before sunrise, and Winslow Whitecrane is already in his driveway waiting for his ride. It’s Thursday morning, his day for dialysis.
He doesn’t dawdle.
“The van pulls up, honks and waits five minutes,” Whitecrane said. “If you’re not out in five minutes, you get left.”
Normally, Whitecrane takes the IHS-provided van to Billings. It picks him up and drops him off at his house in Ashland.
The car makes its way toward Lame Deer to pick up another dialysis patient.
Elrena Whitedirt makes her way out of her home toward the car. She has a canvas bag atop her shoulder filled with blankets, water and food. She’s come prepared for a long day.
“We kind of give each other support to make the trip easier, because me and him always end up getting stuck way in the back of the van,” Whitedirt said.
Whitedirt and Winslow are two of the 30 people from Northern Cheyenne who make the commute.
Enlarge

Whitedirt said the disdain for the commute is universal among the patients.
Outside the capitol building in Lame Deer a fire burned with mounds of firewood next to it. The fire burned for Rock Red Cherries, a tribal chief who had died recently. Killsback said the fire will burn for 2 days so Red Cherries’ spirit can find its way.
Red Cherries was a dialysis patient that made the same commute as Whitecrane and Whitedirt. But the drive wore on him, and he stopped making the trip.
“He could’ve just kept going. He would’ve been still alive today. And there’s a lot of them that happened to,” Whitedirt said. “They all quit going. And they’re gone now.”
Dialysis patients don’t have the luxury of missing a day of treatment or taking a day off. It is literally life or death.
“We have to go no matter what,” Whitedirt said. “No matter what kind of condition it is. We have to go to dialysis.”
While the drive can be physically taxing, those on dialysis who take IHS transportation pay little out of pocket. IHS provides the ride and meals at the end of the day.
Diabetes has proven to be a substantial financial burden on a system that is already financially strained. According to the Department of Health and Human Services, people diagnosed with diabetes have medical costs that are more than double that of a person without diabetes, on average.
End stage renal disease is one of the largest drivers of Medicare costs, according to the National Indian Health Board. In 2009, one patient on dialysis cost Medicare approximately $80,000 a year. Reducing the number of patients on dialysis could greatly reduce the burden on both Medicare and IHS.
The U.S. Government established IHS to provide health care to Native Americans in exchange for the land claimed by the federal government. In efforts to combat the diabetes epidemic sweeping Indian reservations, Congress established the Special Diabetes Program for Indians in the Balanced Budget Act of 1997. At the time, Congress allocated $30 million to fund the program per year. That figure has since increased to $150 million.
~-~
Tammy Roundstone, director of wellness at Northern Cheyenne Tribal Health, a tribally run health clinic, oversees the special diabetes program funding and works with community members with diabetes. She said much of her job, and the job of the community, is about prevention of and education about diabetes.
“I’m not just pushing prevention,” Roundstone said. “I am prevention,”
But she is limited in what she can do in her role at Tribal Health. The facility does not have a doctor on staff, so they have to rely entirely on diagnosis information from the IHS clinic in Lame Deer.
Once a patient is diagnosed, Roundstone steps in to help. She does her best to provide the patient with a sound nutrition and prevention plan, though some don’t follow through with it. Roundstone said some people lose the will to help themselves, and once that occurs, there isn’t much she can do.
Other patients mistake their long-term treatments for cures.
“They stop at McDonalds — which is bad for chronic kidney disease — on the way over, and they stop at McDonalds on the way back. One bun has so much nitrate in it, it throws off their whole dialysis,” Roundstone said. “A lot of them are aware of that. They’ve already lost that concept of ‘I want to help myself.’”
An alternative to dialysis and the commute to Billings is peritoneal dialysis, also known as home dialysis. Instead of traveling to a dialysis clinic and hooking up to a machine, peritoneal dialysis can be done in a patient’s home.
Jay Red Woman, 51, is one of only three home dialysis patients on Northern Cheyenne. Red Woman initially traveled to Billings three times a week, but he couldn’t do it anymore after two months.
Enlarge
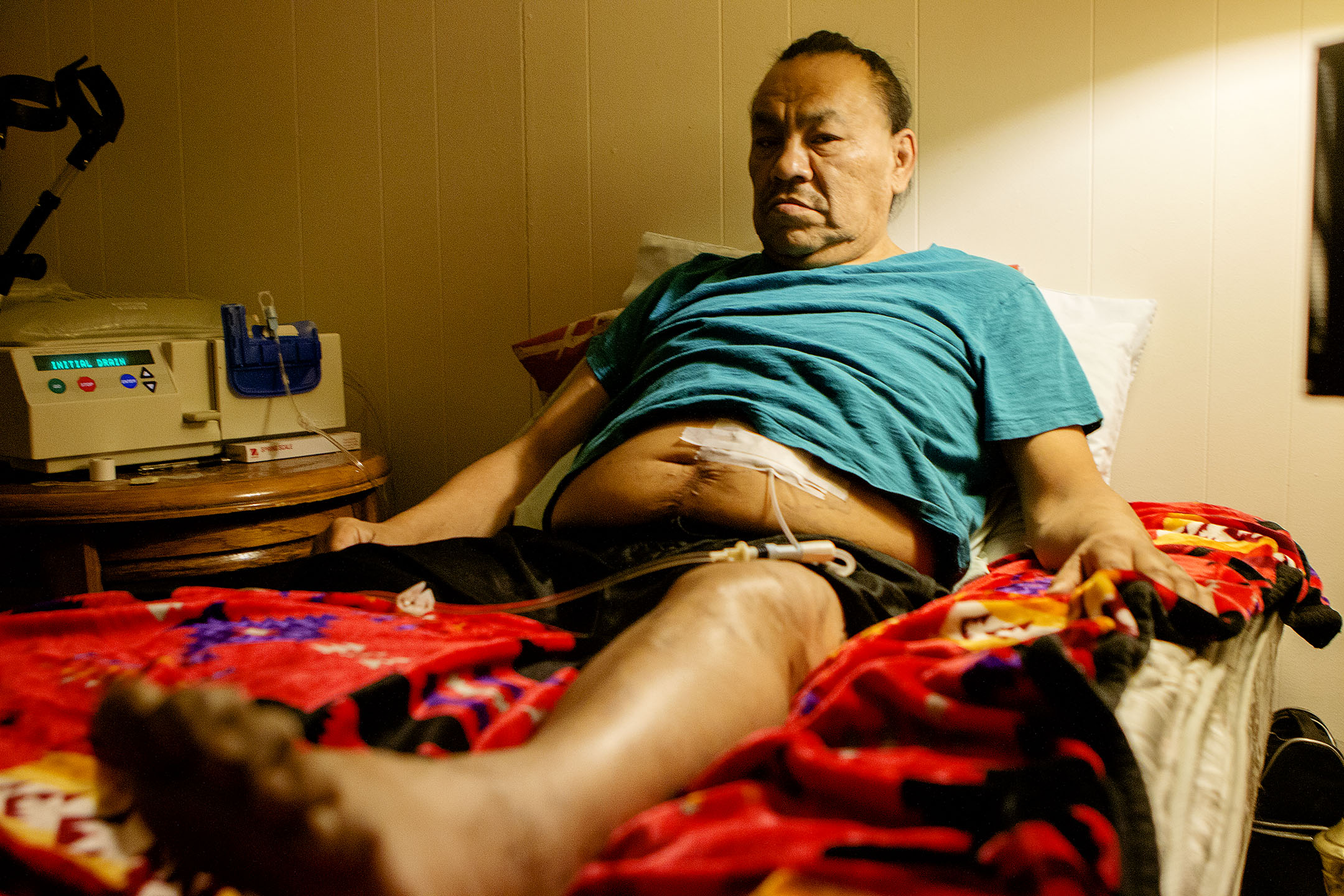
“Every other day, Tuesday, Thursday, Saturday, we’d get up three o’clock in the morning. Alarm would go off like clockwork and get to Billings at about five-thirty in the morning. Get there to that clinic and get in there and I’d be all groggy and they’d hook me up. Over three-and-a-half hours I was on there,” Red Woman said.
Red Woman found out about home dialysis from a nurse, and it immediately piqued his interest.
Vicki Armistead, a registered nurse and training coordinator at Dialysis Center Inc., said home dialysis has been around for a long time, but became popular in the 1960s.
The system works by attaching a catheter to the patient’s abdomen, then using the peritoneum as a filter and solution to clean the blood.
Armistead said a full cycle can take eight to 10 hours to complete. The time required is one of the drawbacks for patients. But Armistead said many patients use it in their sleep.
Armistead said home dialysis offers several benefits to patients beyond convenience.
“Peritoneal is more like natural kidney function,” Armistead said. “They don’t have the ups and downs.”
It also eliminates the need to be near a dialysis clinic at all times.
“I have more freedom and mobility,” Red Woman said. “I can go camping. I just hang up my bag and dwell for an hour. It’s such a relief.”
~-~
With only one prosthetic leg, Old Mouse can’t do everything he wants. In March, he was waiting for the opportunity to prove he could walk 50 feet with a walker and his one prosthetic. In late April, he managed that 50 feet, earning a prescription for his second leg.
“I want to walk outside, mow my lawn and feed my horses,” Old Mouse said. His son currently takes care of the lawn. Old Mouse gave away his horses shortly after his first amputation.
Old Mouse said he will be about 80 percent normal, with his second prosthetic. But as dialysis looms, that’s something he’s struggling with more.
Enlarge

Old Mouse wants a dialysis center in Lame Deer. Like others, Old Mouse views dialysis as a “death sentence” and he’s worried about the toll the long commute will have on every facet of his life.
But for now, Old Mouse is focused on being home and making improvements to his house. He’s making an addition, fitting himself with a larger bathroom to accommodate a wheelchair.
Losing his legs wasn’t something he ever expected, but in the year since he lost them, Old Mouse is adjusting to everyday life, and has come to peace with his legs.
“I’m alright with losing my legs,” Old Mouse said. “I have to be.”
For past Native News editions visit the archive here.









